Information Brochures
Information for Relatives of ICU Patients
This section gives information that should reassure you and let you know where to turn to for help when you need it. A patient may be in intensive care because of an accident, an illness, or for treatment after having a major operation, and relatives and friends will be worried about them. Seeing the patient there for the first time can be very distressing. They are likely to be connected to a number of machines and drips and will often look very different from how they normally look.
-
The early days
Your relative or friend has been admitted to the intensive care unit (ICU) because their body cannot work normally. If they do not get special help, they may have serious long-term effects to their health or they may die. Sometimes patients in an ICU may have to be moved to an ICU in a different hospital. This could be because the patient needs specialist care that is not available. This can be very upsetting for you and you may have to travel further to visit your friend or relative. However, patients are only moved to a different hospital when it is absolutely necessary. When a patient is first admitted to an ICU, it is normal for you to feel helpless, and desperate to know everything you can about their chances of recovery.
However, the patient will need time to let their body rest and get over the shock of becoming so ill. Sometimes they will be given strong pain-killing drugs or sedatives to help the healing process begin. If you have questions about what is being done, ask the staff in the ICU. They will answer your questions as well as they can, but they will not want to give you false hope. The staff will be happy to explain what they are doing and they will be able to update you as time goes on.
-
What can I do to help?
Days may go by with no change in the patient’s condition. There may be nothing for you to do but wait. Nurses will often talk through what they are doing even if the patient is unconscious. This is because, even though they are heavily sedated, the patient may be aware of being touched, but they are unlikely to remember things as clearly as they would when fully conscious.
The nurses may ask you to bring in some of the patient’s personal belongings to help them recover, such as their favourite music. Talking to your relative or friend may also help. Keeping up a one-sided conversation can be difficult, but talking about shared experiences of holidays and good times can make you feel better too. You could also try reading a newspaper, magazine or book to them. Even if the patient is conscious, you may find it hard to communicate with them. If they can’t speak, they may be able to write, or spell out words by pointing to some letters, numbers and common words you have written on a piece of paper.
-
Behaviour
Sometimes, the patient may behave out of character. This may be because of their illness or medication. They may be agitated, confused, scared or paranoid. Paranoia is a form of anxiety or fear that can make you believe people are plotting against you or trying to hurt you. They may also have hallucinations (see things that aren’t really there) and nightmares that seem very real to them. Patients sometimes believe the staff are trying to hurt them. This can be extremely distressing for you and the patient but it will improve as they get better and begin to recover.
If the patient in the ICU has been given sedatives, the sedatives will be gradually reduced as the patient gets better. This process is called weaning. Depending on how ill they were, the drugs they needed and how long they were sedated for, the weaning process can take hours or it can take days. During the weaning process, the patient will be drowsy and confused, particularly in the early stages, but it’s a necessary step and it means they’re getting better.
Where possible, the staff will let the patient and relatives know what treatment options they have. If there is anything you don’t understand or want to know more about, ask the staff. If you’re unhappy with the care being given to the patient and you are not able to deal with this through the ICU staff, please speak with the intensivist who will help you to find the answers you need.
-
Other things you can expect
There may be times when staff ask you to leave the patientʼs bedside. This is because some of the necessary medical procedures are not pleasant and may upset you. It also gives the staff room to do their job.
If the patient is ventilated (on a breathing machine), the nurses have to regularly clear the chest of mucus and fluid. They do this by putting a thinner tube into the breathing tube to suck up the mucus. This is quite noisy and may cause the patient to cough or retch. The fluids given to the patient to keep them hydrated may make them look bloated and swollen. This is normal and will improve as the patient gets better.
Some of the machines that the patient is connected to have alarms that may sound to let staff know that something needs doing, for example if a drip needs to be changed. Usually, there is nothing to worry about – the staff will closely watch the patient at all times.
As we use an electronic medical records system you may find the nurses charting on the computer. This is to upload treatments and monitoring done.
-
Preventing infection
Patients who are critically ill may have difficulty fighting infections and, because of how ill they are to begin with, this can be very serious. The staff will do all they can to make sure the patient is protected. You can help too by washing your hands and using the alcohol hand rubs you’ll see around the unit before you go near or touch the patient. You should also ask other visitors to do the same.
-
Helping the staff
Some relatives find it helpful to be more involved in caring for the patient when they’re recovering. You may be able to help by doing things such as massaging or moisturising their hands and feet. This will depend on how ill the patient is, and won’t always be possible but if you want to help in this way, ask the staff.
It helps if you choose a family member or friend to be the main contact. Staff can tell the main contact how the patient is doing and they can pass on the information to other family members. This will save time for staff and relatives.
-
Looking after yourself
You can help the patient by taking care of yourself. You shouldn’t feel guilty for not being by their bedside 24 hours a day. You need to give yourself a break and this will also give the patient time to rest. The patient will be very well cared for and the staff will contact you straight away if they need to or if there is any change in their condition. Your family and friends will be concerned about you and the patient, and they will want to know how things are. You may appreciate their concern, but it can be tiring if the phone is ringing all the time when you’re at home between visits to the hospital. Passing on the information by e-mail or text message to several people at once can be easier. Or, you could speak to one person regularly and they could pass the information on to others. You may not feel like eating and you may have difficulty sleeping, but do take time to eat regularly and rest when you can. If you become tired and ill, you won’t be able to care very well for the patient.
For family and friends who may be from out of town or live too far away from the hospital we have put together a list of hotels you may choose to reside in to be close. If you require any other assistance please feel free to ask the staff.
Visiting hours for ICUs are usually more flexible than for normal hospital wards, and staff will be able to give you details daily. If you need more support we can arrange counselling, so that you can talk to someone about what has happened. -
Helping children who have a relative in an ICU
For safety reasons, we do not allow young children in the ICU. However, we do know that they may have questions and be confused as to what is going on. You can help a child deal with the situation by:
- Trying to keep to their routine as much as possible
- Telling the school, and any other relevant groups, that the childʼs parent or relative is in intensive care
- Explaining the situation and being honest if you donʼt know what is going to happen
- If you are not sure, try to say something they can understand that will help the child feel secure and reassured, for example, ʻDaddy is very ill but the doctors are doing everything they can to help him’.
Once the patient is out of the ICU, the child may need help dealing with what happened. This can be a gradual process and can take several months. At times, it may be helpful to mention the patients stay in hospital so the child knows they can talk about it. Let them ask questions, and ask them how they felt at that time. If the child is very young, they may find it easier to show their feelings by drawing pictures or acting out what happened. Remember that children can ask very blunt questions, so be prepared.
-
If the patient does not survive
Despite our best efforts, sometimes patients are too ill and do not survive. A person dies when their heart stops beating or they are brain stem dead. If the doctors believe the patient is brain stem dead, they have a set of tests they must follow to confirm this. If the patient has died, the next of kin and family members will be informed. The remains of the patient will be carefully transferred to the morgue which can be decided upon by the family. We will always be there to support you and your family during this difficult process, should it occur.
Day Case Information
A day case is an elective procedure which will be done on the same day of admission and the patient will be discharged home on that same day. This information brochure helps you plan for the procedure and gives you information on about what to expect.
Before the day
- You will be reviewed by the health assessment clinic and necessary investigations done.
- It is advisable not to drink alcohol for at least 24 hours before your operation.
- It is also advisable to quit smoking where possible, weeks prior to surgery.
How do I prepare for my operation?
- You must arrange for a responsible adult to accompany you home, and to stay with you for 24 hours following your operation. You must contact the hospital at least 48 hours before your admission if you are unable to arrange this. The type of surgery that you have may require you to have an overnight stay. In normal circumstances, you will be informed of this at your preoperative appointment.
The night before
- If you are having your operation under a local anaesthetic, you can eat and drink as normal prior to your admission.
- If you are having your operation under any other anaesthetic it is very important that your stomach is empty before your operation. It is not necessary to starve for longer than the times given below as doing so may cause general discomfort and may delay your recovery.
If you are having your operation in the morning:
• Do not eat anything after 3am – this includes chewing gum and sweets
• You may drink clear fluids up to 7am – examples of clear fluids are water, tea and coffee without milk, sugar or sweetener.
If you are having your operation in the afternoon:
• Do not eat anything after 8am – this includes chewing gum or sweets; you may have a light breakfast of toast or cereal before this time
• You may drink clear fluids up to midday – examples of clear fluids are water, tea or coffee without milk, sugar or sweetener.
The day of surgery
- Come in early. An arrival time will be communicated to you.
- Wear comfortable, loose-fitting clothes that you can also travel home in.
- Please have a bath or shower before your admission.
- If you have been given any products at your preoperative assessment please use these as directed.
- Make-up, nail varnish and any piercings must be removed.
- Take your regular medication on the day of your admission at your usual time unless informed not to do so at your preoperative assessment.
After the procedure
- You should be discharged from the Day Case Unit in the same 24-hour period as your operation.
- Arrangements will be made for any follow up treatment or appointments you may require.
- Information following your surgery will be given to you before leaving the hospital, including care of wounds.
- You will be prescribed additional pain relief if it is required.
- You must not use public transport or drive yourself home.
- If you require a sick note, please inform the nurse on admission.
We will advise you on when you can go back to work and when you can resume driving.
Recovery at home
It is important to rest for a few days after your operation, especially if you feel sick or dizzy. For 24 hours after your operation you must not:
- Operate machinery or domestic appliances including cookers, kettles and irons.
- Drink alcohol or take sleeping tablets.
Please ensure you keep your next clinic appointment and let the nurse know if the date given isn’t convenient so we can change it.
IN CASE OF EMERGENCY
If you begin to feel unwell come right back to the emergency room to see a doctor.
What is Colorectal Cancer?
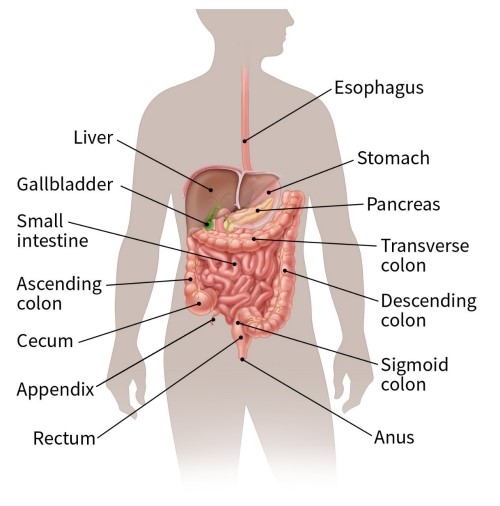
Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). It has become more common but unlike some malignant tumors, colorectal cancer can often be cured by surgery, and new treatments are being introduced to make survival even more likely. The earlier the colorectal cancer is diagnosed, the greater the likelihood of cure.
How does a polyp turn to cancer?
It often begins as an abnormal growth called a polyp, which could then become malignant, or cancerous. It could then spread to nearby tissues and more widely throughout the body, particularly to the liver and the lungs. When cancer spreads far away from its primary site (in this case the bowel) to distant parts of the body, it is said to have metastasized.
What are the symptoms of colorectal cancer?
common symptoms are;
- Blood in stool
- Change in bowel habit- such as unusual episodes of diarrhea or constipation, mucus in the stool.
It can enlarge so that it partially or completely blocks the bowel leading to abdominal pain, constipation, and bloating. This is very bad.
What tests should be done?
Sometimes, the doctor will be able to detect a lump in the abdomen or on rectal examination but usually tests are needed. The most commonly used is:
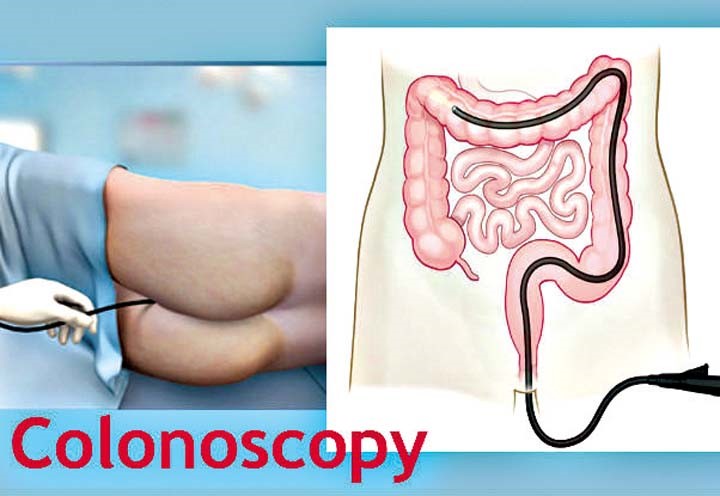
Colonoscopy—A flexible telescope is passed through the anus into the rectum but the tube is long enough to examine the entire large bowel. The procedure can be a little uncomfortable and so patients are given drugs to ease any discomfort. If any lump is seen, a small sample or biopsy can be taken to look at under the microscope.
What happens once cancer is diagnosed?
If you are found to have colorectal cancer, a team of specialists is there to help. You will be advised to have blood tests and scans to determine what is known as the stage (extent) of the cancer. Not only will the size of the primary tumor be assessed thoroughly, but the specialist will also want to know if there is any sign of secondary spread. Armed with all the relevant information they have gathered about the cancer; the specialists will decide how best to advise you on the most appropriate treatment.
How are cancers of the colon and rectum treated?
Once tests have confirmed that the cancer has not spread anywhere else, most colon cancers are treated by surgery. ftis will usually involve removing the cancer together with the lymph glands along the blood vessels supplying that section of the bowel. In most cases, the two ends of the bowel are joined together again (anastomosis) but if the cancer has led to an emergency, it may not be possible to join the bowel together right away. Once the colorectal cancer and surrounding tissue have been removed they will be examined.